Declining childhood vaccination and federal policy signals raise short‑term risk of vaccine‑preventable disease resurgence
Thesis: Reported declines in routine childhood vaccination—combined with recent federal advisory signals and public debate about immunization guidance—have increased the short‑term risk that measles and other vaccine‑preventable diseases will reemerge in vulnerable communities.
Executive summary — what changed and why it matters
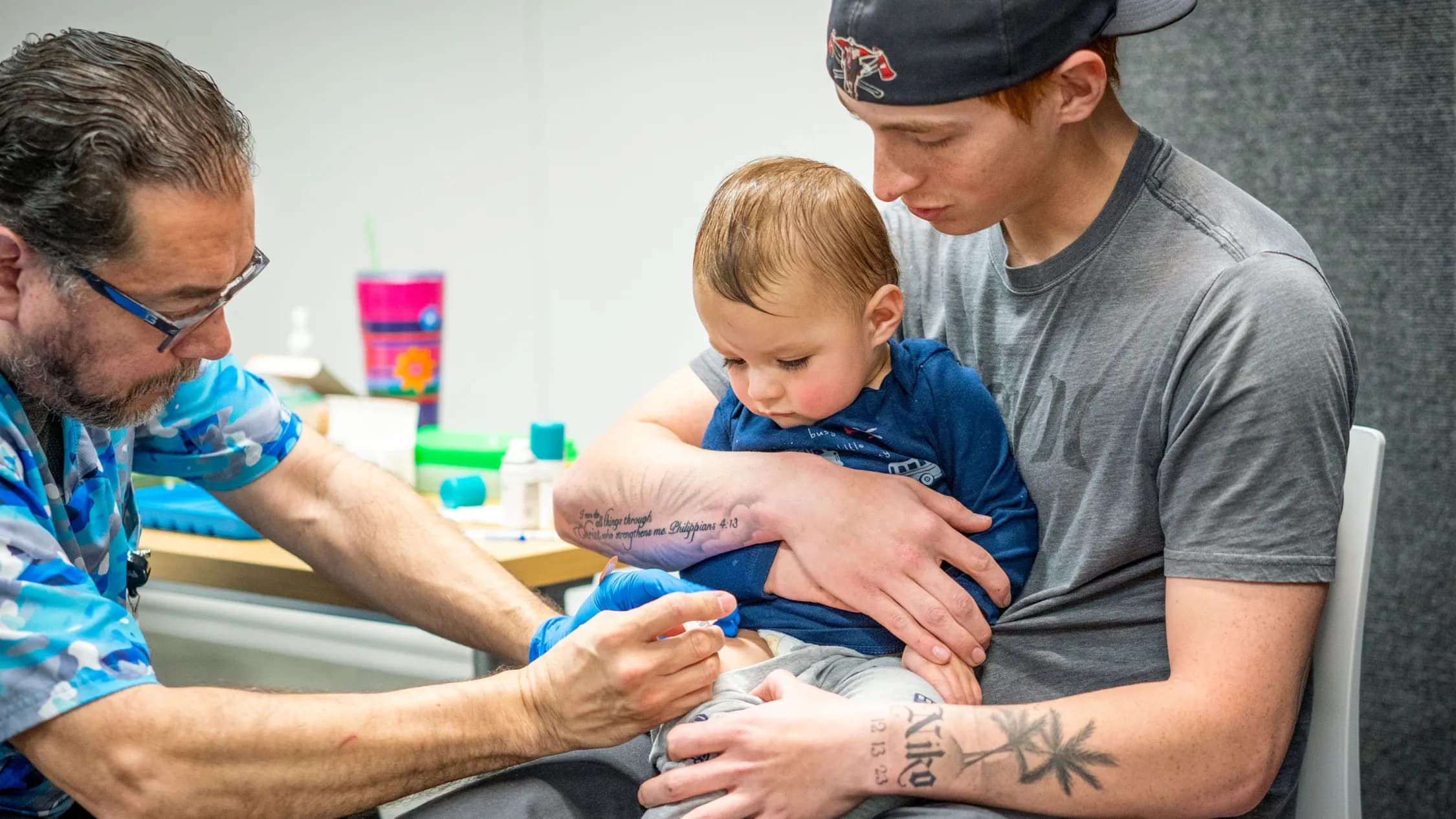
Public‑health reports from multiple jurisdictions describe a clear pattern: pockets of under‑vaccination are permitting highly transmissible infections such as measles to spread again, and contemporaneous uncertainty in federal advisory messaging is amplifying operational and perception risks. Local reports cite confirmed measles clusters this year (for example, 34 cases in Enfield, north London, since January 2026 and 962 cases reported in South Carolina since October 2025), with larger outbreaks described in several U.S. states; these figures are reported by local authorities and media and should be verified against national surveillance data.
- Impact now: Measles transmission is occurring in low‑coverage pockets and reported hospitalizations have followed (local reports indicate about one in five Enfield cases required hospital care; verification needed).
- Vaccination gaps: Jurisdictional data cited to date show kindergarten two‑dose MMR coverage falling from the mid‑90s to the low‑90s in some places and much lower in specific schools or boroughs; those local coverage figures are reported by public‑health offices and school records and merit validation.
- Near‑term risk: Measles’ high transmissibility makes it a bellwether: sustained local drops in MMR uptake increase the likelihood that other vaccine‑preventable infections—mumps, rubella, polio, hepatitis B—will find susceptible hosts.
- Policy and perception risk: Reporting about changes or debate in federal vaccine guidance—including coverage of newborn hepatitis B recommendations and public discussion of polio guidance—has added ambiguity around clinical practice and given pause to some providers and parents (reports vary by outlet; statements from agencies should be consulted for confirmation).
Breaking down the data
The epidemiologic signal is characterized less by a single nationwide trend and more by clustered vulnerability. Measles requires roughly 95% two‑dose population immunity to block sustained chains of transmission; where coverage dips into the low‑90s or below, susceptible cohorts large enough to sustain outbreaks can appear.
Local surveillance data and school‑level records highlighted in recent reports show pronounced heterogeneity: some districts report broadly adequate uptake, while others report coverage that public health officials characterize as far below herd‑immunity thresholds. Where those low‑coverage pockets overlap with social vulnerability—limited access to care, linguistic isolation, or distrust of institutions—the potential for rapid local spread rises.

Because many of the numeric claims circulating in media summaries and local briefings are drawn from varied sources (school registries, local health department case counts, press statements), the provenance of any single percentage or case total should be treated as indicative rather than definitive until matched to national or peer‑reviewed data.
Why this could presage other vaccine‑preventable disease increases
Declines in routine childhood immunization do not only affect measles. MMR uptake is linked epidemiologically to control of mumps and rubella; lower coverage increases population susceptibility to those pathogens and to complications that can be severe for some individuals. Separately, changes in acceptance or delivery of hepatitis B or polio vaccines—whether driven by policy shifts, supply constraints, or erosion of public confidence—create independent pathways for resurgence.
Historical precedent underscores the speed of such reversals: previously controlled pathogens have recurred in under‑immunized communities, as public reporting around events such as the 2022 paralytic polio case in New York has highlighted. Some consequences, like measles encephalitis, are acute; others, such as chronic hepatitis B leading to liver disease decades later, carry intergenerational and long‑term health impacts.
Policy signals, ambiguity, and human stakes
Federal advisory ambiguity—or even the perception of ambiguity—has human consequences. When national guidance is reported as changing or debated, clinicians confront practical uncertainty about standard practice, parents encounter conflicting messages about risk and benefit, and communities with existing mistrust of healthcare institutions can see that mistrust deepen. Those dynamics reorganize power and agency: who decides which children get protected, which clinics receive resources, and which communities are prioritized for outreach becomes politically and socially charged.
The current mix of local outbreaks and public discussion about federal guidance raises three linked risks: operational strain on clinics and hospitals in surge scenarios; widening inequities if low‑coverage pockets coincide with marginalized populations; and an expanded information ecosystem in which ambiguity fuels hesitancy narratives.
Likely jurisdictional responses and trade‑offs
Rather than a prescriptive checklist, the observable responses and tradeoffs fall into patterns. Some jurisdictions are reported to be intensifying targeted vaccination outreach and school‑based catch‑ups; others are prioritizing surveillance and genomic sequencing to understand transmission. These choices involve political and resource tradeoffs: redirecting staff to surge immunization can strain routine services; aggressive public messaging can prompt political backlash in polarized settings; and programs that improve access in one community may not immediately rebuild trust in another.
Agencies balancing these options face dilemmas about visibility versus persuasion, rapid short‑term containment versus sustained investment in primary care, and legal authority versus community consent. Those tradeoffs will shape which communities experience repeated outbreaks and which regain stable coverage.
Conclusion
Reported declines in routine childhood vaccination, layered over current federal advisory ambiguity and public debate, present a coherent near‑term pathway for the return of vaccine‑preventable disease in vulnerable communities. The stakes are human: preventable illness, lost trust in institutions, and long‑term burdens that fall unevenly across populations. Key numeric assertions in current reporting should be verified against official surveillance datasets, but the diagnostic signal—localized immunity gaps plus policy uncertainty—should be treated as a credible short‑term risk vector for resurgent infections.